Rescue Squad Adopts an Intuitive CAD Solution To Ramp up Dispatch and Improve Data Visualization
What Were the 12 Hottest Topics in EMS in 2017?
Because the holiday season is in full swing, I was tempted to begin this blog post with one of my favorite Christmas clichés (think: a cheesy parody of The 12 Days of Christmas…) to tee up this Top listicle, until I read this article about how any writer with a modicum of self-respect should never, never, never use them in copy or headlines.

Because the holiday season is in full swing, I was tempted to begin this blog post with one of my favorite Christmas clichés (think: a cheesy parody of The 12 Days of Christmas…) to tee up this Top listicle, until I read this article about how any writer with a modicum of self-respect should never, never, never use them in copy or headlines. So we’ll kick off with a much more traditional opening – however, I’m sticking with the number 12 just because I'm feeling festive and I think it sounds more holiday-like than 10 – to introduce the 12 hottest topics to EMS providers in 2017.
It turns out that four out of 12 of our most viewed blogs posts this year were on how to improve your patient care reports. What other topics resonated well with our audience? Here's our most popular content from 2017, which can be used as great resources to help polish off your 2018 plans:
Taking a Deeper Look at the Guidelines for CPR
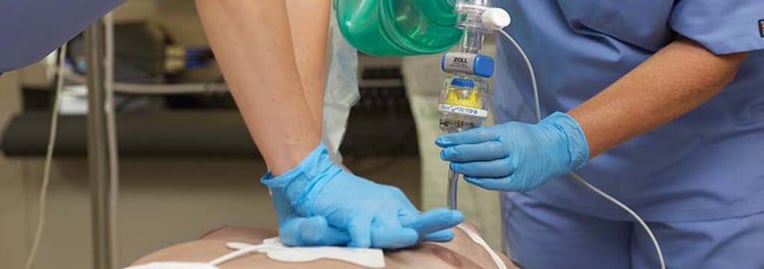 Not too long ago, all you need to ensure you are doing good chest compressions is to push hard and push fast. In 2015, the American Heart Association Guidelines have raised the CPR bar. Now, there is a greater specificity on the rate and depth of compressions; and we need to meet these targets if we want more patients to survive and ultimately be discharged from the hospital.
Not too long ago, all you need to ensure you are doing good chest compressions is to push hard and push fast. In 2015, the American Heart Association Guidelines have raised the CPR bar. Now, there is a greater specificity on the rate and depth of compressions; and we need to meet these targets if we want more patients to survive and ultimately be discharged from the hospital.
Why Measure the Quality of Resuscitation? LA County Fire Department Shares Their Journey, Lessons Learned
One of the largest fire departments in the United States, the Los Angeles (LA) County Fire Department has 174 fire stations, 73 paramedic squads and many more paramedic assessment units. It services an area of 2,300 square miles that includes all unincorporated parts of LA County and 58 contract cities, all of the county’s beaches except Long Beach, and Catalina Island. It even includes air operations, with eight helicopters – three are in service at one time with a fourth in reserve. In 2016, LA County Fire Department’s call volume was approximately 350,000. Of those calls, 300 to 350 calls per month are for cardiac arrest. How could CPR performance and patient outcomes improve if the fire department started collecting and analyzing data on those calls?
EMS Mobile App Roundup – Check Out the Latest & Greatest
 Mobile apps are changing the way EMS providers operate in the field. We’ve rounded up some of the most useful EMS apps to help improve the quality of CPR, locate the nearest AED, record patient care information on your phone and more.
Mobile apps are changing the way EMS providers operate in the field. We’ve rounded up some of the most useful EMS apps to help improve the quality of CPR, locate the nearest AED, record patient care information on your phone and more.
Paint a Complete Patient Story to Eliminate Denied Claims
A good narrative clearly documents the patient’s response to the treatments provided. In other words, as a result of the treatment, did the patient’s condition improve, and if so, how? To a great extent, crews should see checkboxes and dropdown lists throughout their PCR as reminders of the various aspects of this patient’s care that need to be more fully developed and clearly documented in the narrative. Quality, not quantity should be the goal.
5. The Community Paramedicine Payment Evolution
 As community paramedicine (CP) evolves, so does the approach to payment of services. It appears that payment is going in two directions. The first type of payment is a more traditional, fee-for-service model with which the ambulance world is familiar. The second approach to payment will help sustain and grow CP programs, but doesn’t work well with our conventional billing and tracking systems. This isn’t an insurmountable problem as new systems are also evolving. Today, we talk about the progress of CP payment models and what providers need to do to get paid for these growing, essential services.
As community paramedicine (CP) evolves, so does the approach to payment of services. It appears that payment is going in two directions. The first type of payment is a more traditional, fee-for-service model with which the ambulance world is familiar. The second approach to payment will help sustain and grow CP programs, but doesn’t work well with our conventional billing and tracking systems. This isn’t an insurmountable problem as new systems are also evolving. Today, we talk about the progress of CP payment models and what providers need to do to get paid for these growing, essential services.
6. 7 Essential Elements for a High-Quality Patient Care Report
As healthcare professionals, it’s our responsibility to ensure that our documentation of patient interaction is documented appropriately. What does that mean? Be sure to include these components for a complete narrative.
7. 6 Dashboards to Improve Clinical Outcomes
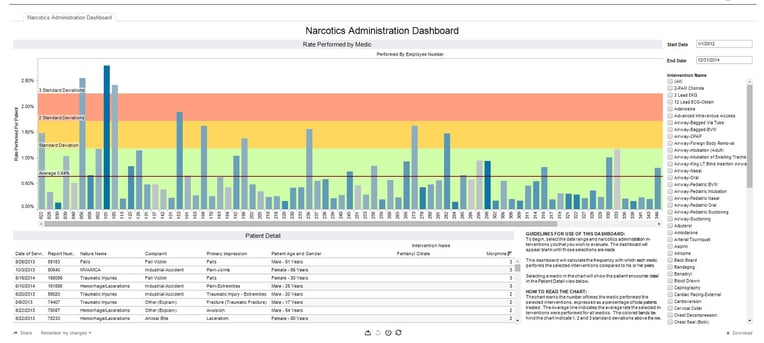 Until recently you had to be a spreadsheet wizard, Crystal Report guru or hassle the IT department to access and make sense of your data. Advancements in technology have empowered improvements in the ability to collect and process large volumes of data. Software service providers have responded with enhanced reporting capabilities that incorporate charts and graphs (visualizations) to simplify the ability to identify trends and measure performance.
Until recently you had to be a spreadsheet wizard, Crystal Report guru or hassle the IT department to access and make sense of your data. Advancements in technology have empowered improvements in the ability to collect and process large volumes of data. Software service providers have responded with enhanced reporting capabilities that incorporate charts and graphs (visualizations) to simplify the ability to identify trends and measure performance.
8. Keys to Better Billing Management
Actions in dispatch, the field and billing will improve operating efficiency and have a positive impact on cash flow. Follow these steps to improve operations and get paid for transports.
9. Building an Efficient, Yet Lean EMS System
Last May, ZOLL recognized several professionals for being the pulse of their organization by providing better care and enabling their teams to save more lives within their community. Alexander Lewinsky has been instrumental in growing JFK EMS and has tirelessly worked to improve the agency’s systems.
10. Documentation Compliance in the Real World
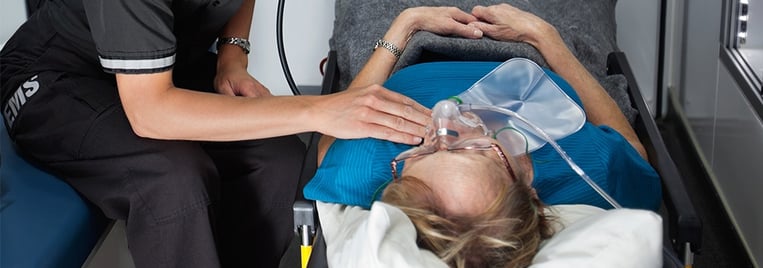 Did you know there’s a chance your agency may not get reimbursed because of poor documentation? Teach crews why they document and how their documentation is related to the patient for more thorough trip reports.
Did you know there’s a chance your agency may not get reimbursed because of poor documentation? Teach crews why they document and how their documentation is related to the patient for more thorough trip reports.
11. How Florida Hospital Closed the Divide Between Air & Ground EMS
Despite making strides to change our culture, we had several minor accidents, speeding tickets and red light violations. We even had fairly serious accident that was fortunately without fatalities where an SUV T-boned one of our ambulances with a patient on board in an intersection. Several other events caused us to pause in order to determine what was missing. We realized what we didn’t have was real-time data that could paint a picture of how our crews were actually behaving on the road. We did our homework, and identified Road Safety as the missing link in our culture of safety program. When we saw the data from Road Safety, I was absolutely shocked at the number of violations that were occurring as our crews were on the road.
12. Bloomington Hospital EMS Tried a Competitor of Road Safety for 1 Year; Find Out What Happened
 Not only did Road Safety help us protect our drivers in those two examples, we used the data in the reports to develop new driver policies. Last but not least, we also spent less on maintenance, insurance and repairs for our fleet. So why did we move to a competitor system in 2016?
Not only did Road Safety help us protect our drivers in those two examples, we used the data in the reports to develop new driver policies. Last but not least, we also spent less on maintenance, insurance and repairs for our fleet. So why did we move to a competitor system in 2016?
Related Posts
Christa Lassen-Vogel, Senior Manager, ZOLL Data Systems | Mar 12, 2024
EMS-to-Hospital Handoffs Can Be a More Streamlined Experience
ZOLL Data Systems | Jan 25, 2024
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS, fire, hospital, or AR professional easier.
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS, fire, hospital, or AR professional easier.



